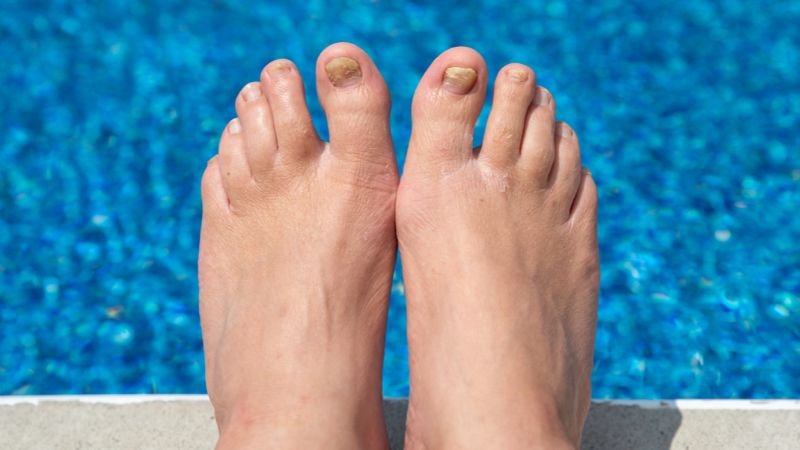
Help Treat Fungal Toe Nails with Coconut Oil
Coconut oil contains natural antifungal compounds, including lauric acid and caprylic acid, which may help fight the organisms responsible for fungal toenails. It also helps moisturize and protect the nail…